
Advisor Blog | Oct 2021
The COVID Crisis One Year Later: Revisiting Healthcare Board Director and CHRO Perspectives
A recap of recent conversations with healthcare leaders about emerging solutions to their organizations’ current challenges.
In 2020, just after the onset of the COVID-19 crisis, Pearl Meyer conducted two healthcare peer exchange sessions. One included CHROs and the other included health system board members. We provided a forum for participants to come together and discuss the challenges their organizations were experiencing and share ideas.
A full year later, we decided to revisit the concept to learn about the manner in which provider organizations have adapted to the ongoing pandemic and to better understand the new challenges that are present. It was clear from the beginning of these discussions that last year’s challenges have evolved. Some were expected, such as burnout, and others less expected such as the impact of new competitors both inside and outside the industry driving up wages. And of course, the “Great Resignation” is marked by broader individual reconsiderations about safety, mental health, work-life balance, the ability to work remotely, and finding renewed purpose in the face of loss, among a host of other reasons. This well documented trend is hitting the healthcare industry particularly hard.
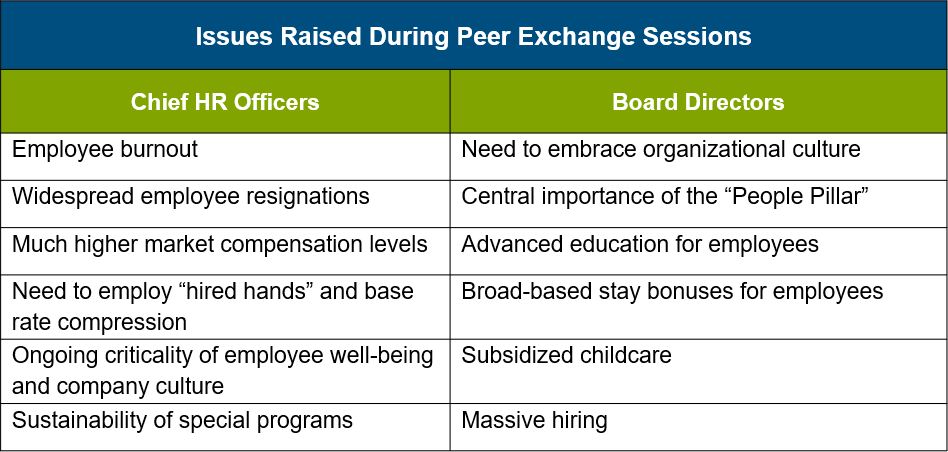
These disruptions are having—or will soon have—detrimental effects on the ability of health systems to provide the right care at the right time consistently. It is all further complicated by the fact that the delta variant has been pulling us closer to the height of last year’s pandemic than to full recovery. In the face of these circumstances, both the CHROs and board members in our discussions underscored the strategic and operational importance of embracing culture and people in order to sustain their ability to provide quality patient care, successfully ride out the still-evolving pandemic environment, and thrive in the future.
The following three major themes emerged during our two peer exchange sessions:
Labor Market Challenges
The CHRO of one 16-hospital academic health system, which is spread across three states and driven by 30,000 employees, encapsulated the issues that the others in the conversation quickly signed onto: They have a perfect storm of losing talent in places that were unexpected, not being able to hire quickly enough, and skyrocketing turnover, particularly with RNs. (They also noted the RN scarcity even before the pandemic.) These challenges are seen across the continuum of roles and positions, for example, food services, environmental services, back-office operations, HR, CRNAs, and new roles such as DE&I (Diversity, Equity, and Inclusion) where the talent pool itself is relatively new and slim.
Panelists shared that these staffing challenges among clinical staff, and specifically RNs are being driven by burnout from the inhumane schedule over the past year as healthcare workers poured all they have into caring for the COVID and non-COVID patients alike for the sake of their communities, and also by the allure of increased compensation, if willing to travel.
It became clear during the conversation with the CHROs that traditional compensation approaches, such as market-based pay premiums for additional shifts, are not working. One CHRO shared “When a nearby company increases environmental services staff compensation to $18 an hour and you are considering a move to $15 an hour, you find yourself at a significant disadvantage.” In addition, all agreed that candidates starting salary requests have increased dramatically which presents internal salary compression considerations for existing staff and its effect on morale. Moreover, it is important to not gloss over non-clinical staff because it is worth remembering that if hospital rooms cannot be cleaned, infection rates may increase, quality is negatively impacted, and patient experience is diminished.
Non-Traditional Approaches
A number of non-traditional approaches were described by board members which align with what Pearl Meyer is hearing among the firm’s healthcare clients. Leadership assessment and development efforts are also picking up speed at many health systems. While these initiatives are not new to healthcare, their implementation across lower levels of management is non-traditional. The premium of retention is forcing executives and compensation committees to begin considering succession planning and development efforts among mid-careerists. Non-traditional compensation arrangements are sometimes an additional part of these investments in future leaders in the form of incentive pay arrangements.
One of the peer exchange board members detailed his organization’s decision to double down on supporting employer-subsidized advanced education for employees. The idea is that the advanced degree or credential could provide opportunities for employees to consider new roles, which could alleviate their sense of burnout and recognizes the value of that individual to the health system. This serves multiple aims including future opportunities and earning potential for the individual, and fulfillment of the health system’s future needs. The same organization also created a child development center to assist with childcare. While not cost free to the employee, the program follows a three-tier subsidized model based on income to make it more attractive and affordable. These initiatives have had a direct impact on the organization’s ability to retain clinical and non-clinical staff.
In addition, bonuses were paid to staff across the board if they remained with the system for the entire fiscal year, and margin was sufficient. At the time of our discussion, the system was two points above target for the bonus to be realized, representing bonuses worth over $20m. These approaches were initiated simultaneous with one other—a massive hiring initiative to address what has been growing emergency department and ICU patient volumes and the widespread loss of employees, alleviate staff burnout, and bolster the organization’s ability to add more part-time employment packages.
All of these steps, particularly the arms race towards higher compensation to address immediate staffing needs, begs another significant concern expressed by the seasoned CHROs and board members: How can their organizations pull back these enhancements, assuming the environment subsides, because the cost model is not sustainable for the organization. The growing perception among our participants is that these types of programs may not be temporary particularly when coupled with a growing shift toward more “livable wages” which existed prior to the pandemic. Several of the board member participants stated that this continued upward cost spiral will drive an accelerated rate of industry consolidation based on the need for economies of scale.
Ongoing Consolidation
That same concept of achieving economies of scale drove at least one of the participating health systems to form an alliance with a much larger national healthcare franchise. One of the board members described their organization’s desire to quickly, reliably, and cost effectively ensure they were following best practice guidelines and were raising quality “a level or two.”
Our participating HR leaders expressed the notion that “the issues will remain” once the impact of enhanced unemployment benefits subside. They all stressed the importance of continuing to focus on well-being and culture in order to create a welcoming and motivating atmosphere that values individuals, their contributions, and the lives they lead after work. Those healthcare workers wishing to stay in the industry are now, more than ever, searching for the environment that focuses on the quality of care they can provide as opposed to what feels to them as crushing volume expectations.
One CHRO asked whether the continued growth in ambulatory care, home health, and other peripherals will fill the reduction in the delivery of traditional acute care services left by the pandemic. Another questioned whether pre-pandemic striving for the “Triple Aim” has caused health systems to lose their way by over-focusing on productivity and efficiency and losing the little touches (personalized scrubs, lunches, coffee, a slower pace) that maintained engagement and which is now more front and center.
Board members and HR leaders alike wondered whether administrative technologies such as advanced ERP systems help lessen the burden and allow for better information flow and real-time data to enhance decision making so less time is spent on getting to the outcome and more time is focused on addressing the outcome. Even if that is the case, the huge investment required to implement such systems is not one that many organizations can make. As one-click transactions become the norm in our society, the relatively antiquated processes in place within most health systems won’t just drive healthcare consolidation, but rather widespread cross-industry integration.
Summary
Both the board members and CHROs with whom we spoke are obviously focused on addressing the immediate pandemic-related concerns, but also very much focused on the future trajectory of their systems. Top of mind is how to expand beyond geographic growth and include improved outpatient settings, further expansion of telehealth, meaningful clinical affiliations, and more.
Board members sounded more optimistic about the future than CHROs, not altogether surprising given the two groups’ different perspectives. Even so both groups acknowledged the importance of coupling competitive compensation with an attractive culture and individual employee recognition and professional development programs. Provider organizations must make decisions to best play the hand they have been dealt and these decisions will set the stage for tomorrow’s challenges—whatever they may be. Watching from the sideline is not an option.
